Basic Knowledge You Need to Plan for the Rest of the COVID-19 Pandemic
There are a few basic notions that have changed since the beginning of the pandemic. They are important to understand as a basis for thinking about and planning for your approach to what's next. The Delta variant has really changed the entire game. In March 2021, I thought that we could see the light at the end of the tunnel, at least for the US. I started canceling my pandemic supply subscriptions, thinking that I had enough. In May, after following the alpha (UK) variant, I presciently advised the person I was vaccinating to plan their long-awaited travel to see family in June because I can't predict low case counts through July as more variants evolve. Now, I see that we are at best half way through the pandemic, and that until most of the world is vaccinated, we cannot stop paying attention to this virus. We are heading into another self-directed lockdown for our family, as Delta sweeps through. This time, we have much more data on which mitigation measures are most effective.
Worry more about the air than surfaces.
We no longer have to worry as much about contracting the virus through surfaces. Takeout food is quite safe (especially heated items), as are most items at a grocery store that someone else might have handled. I’ll still wipe my cart and sanitize my hands after shopping or putting away delivered goods. With the Delta variant taking hold of my local community, however, I might begin to spray down my cold/frozen foods again with alcohol, since viruses survive longer there. I'll probably begin this soon as our county surges from substantial transmission (50-100 cases per 100,000 people in a week or a positivity rate of 5-8%) to high transmission rates (over 100 cases per 100,000 people in a week or a positivity rate of over 8%). You can check your county’s transmission levels at the CDC website.
The real problem is with the air. Don't share the same airspace with too many people for too long. My previous rule of thumb was to avoid sharing the same air with a potentially infected person (which could be anyone) for 15 minutes, which seemed fine at the beginning of the pandemic and particularly after vaccinations were available to everyone and while everyone was still masked. Now transmission is possible within seconds. That really changes types of “safe” interactions. The viral load with Delta is over 1000 times higher than with the original virus for the first six days whether or not the person is vaccinated. That means that the air exhaled by a contagious person will contain many more infectious particles. If the contagious person is in an enclosed environment with stagnant air, there will be viral particles floating in the air as soon as you enter that person's air space, whether or not they are wearing a mask. Unless you are wearing a well-fitting N95 mask, you won't be well protected.
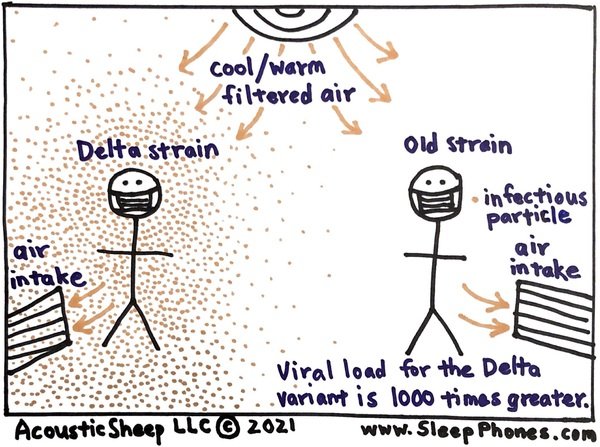
Do masks still help? Yes, in passing interactions, such as at a grocery store, non-N95 masks (such as cloth or surgical) worn by an infectious person still help reduce droplet transmission. It won’t help as much with aerosols that can easily pass through the pores of the mask, but it takes time to breath in enough aerosols to get infected. In a passing interaction, such as the 10 seconds it takes for you to pick out tomatoes while wearing a cloth mask, you are unlikely to breathe in enough infectious particles to cause disease. That's why masks are back. If you have access to high quality surgical or N95 masks that fit well, now is the time to use them, particularly for indoor situations to protect yourself, as well as others from you, just in case you are unknowingly contagious. Unless you are in healthcare or have a possible exposure, you can reuse masks. In the early days of the pandemic when there weren’t enough masks, some healthcare workers would put their used N95 masks into a bag and wait a week to reuse them. The theory is that any germs on the mask would be inactive in a week.

With schools opening a few weeks from now and the Delta surge sending more kids than ever into hospitals, everyone wearing masks in schools is a no-brainer. Even vaccinated teachers can still spread the virus to the kids, and a mask mandate is far easier to enforce if there are no exceptions. Teachers need to set a good example, and wearing a mask will help children follow their lead. Masks will definitely keep schools safer, but virtual school should be an option as well when cases are high in an area. When our county hits high transmission levels (over 100 cases per 100,000 people in a week or a positivity rate of over 8%), I will be shifting my employee work schedules again and keeping my young unvaccinated kids home. I’ll also be keeping a couple of quick home COVID-19 tests around to help with decision making if someone doesn’t feel good. They aren’t as accurate as the PCR tests, but they are much faster. At $20 for two tests, they are likely worth it, considering opportunity cost. The high transmissibility of the Delta variant requires us to constantly re-evaluate and shift our plans.
Wishlist for Schools (not comprehensive)
- Masks are mandatory for everyone, including vaccinated staff. Surgical masks are better than cloth and usually more comfortable.
- Lunch should be outdoors if possible. Otherwise, reduce the number of kids in the lunchroom at a time, clean between groups, and keep them as physically distanced as possible. Minimize the time allowed for lunch. If a student finishes eating, they may return to their classroom rather than remaining in a room with unmasked classmates.
- Integrate a virtual option so quarantining students can remain home and still keep up with classwork and other classmates. Staying home should be neither a punishment nor a reward.
- Cohort students so that quarantines would involve smaller groups.
- Work with HVAC experts to maximize the air exchange in a classroom and understand the air flow dynamics in a classroom when the doors and windows are closed, when the door is open, when windows are open, or any likely combinations.
- Even if a room is not being actively cooled or heated, a fan should be constantly running to keep up the fresh air exchange.
- Include COVID-19 vaccine when approved into the routinely required vaccines.
In fact, this pandemic has caused a sea change in the long-held dogma of fomites and coughing spreading germs. In 1962, a rigid dividing line was established between droplets and aerosol or airborne transmission. It was believed that most viruses spread through droplets. Droplets are defined as particles over five microns in size, which fall to the ground with gravity within three to six feet. (A human hair is 70 microns in diameter.) Droplets land on surfaces such as hands and stick to door knobs. Aerosol transmission particles are less than five microns in size and can stay suspended in the air and drift along air currents for hours. An air pollution scientist, a historian, and a chemist helped to debunk the five micron “rule” during this pandemic.
This firm line between droplets and airborne diseases held back face mask recommendations early on because many scientists still believed that droplets landing on surfaces, fomite transmission, direct coughing/sneezing were the main causes of spread. While they certainly play a role, we did not fully recognize the importance of airborne transmission quickly enough. The WHO finally updated their guidance to include aerosols in May 2021. The policies from the CDC, WHO, and many other organizations did not recognize enough airborne spread, and they are still not recommending enough aerosol mitigation measures.
The six feet rule is an effective idea for droplet precautions, as are double layered cloth masks. But COVID-19 spreads by both droplets and aerosol particles. Sitting six feet away from someone is inadequate for an airborne disease. Airborne particles accumulate and linger in the air based on the amount of time someone spent breathing there, with or without a mask. To clarify, masks of all types still help reduce transmission risk significantly. But with Delta, simple cloth masks are no longer enough. A contagious person exhales so much more virus in each aerosol particle which passes right through cloth masks. As I mentioned above, just seconds of sharing air is now enough for transmission compared with 15 minutes with the original virus. Plus, the Delta variant sidesteps the vaccine and still infects vaccinated people who are just as contagious as a non-vaccinated person in the first six days.
Rather than counting on the six feet rule to protect you, it may be more effective to visualize each person in a room shooting a glitter cannon above their head every single minute. If you are downwind of someone, you may end up with more glitter than if you were upwind. If there are more people in a room, there will be more glitter floating around. Even if you are on opposite corners of a room from someone else, if you are in the room for long enough, you will be glittered. The more glitter you accumulate, the more risky a situation.
As an aside, the debunking of the droplet versus airborne theory has led to a more nuanced approach for understanding how the flu virus spreads too. We skipped the 2020-2021 flu season because many of us stayed distanced during the holidays and wore masks. The transmissibility of the flu actually isn’t super high normally. With the swine flu from 2009, one person would only transmit to 1.5 others. When we were locking down during the 2020 holiday season, COVID-19 was transmitting at a rate of one person to two or three people. Because we were trying to suppress a more contagious virus, we managed to also contain many other viruses with lower transmissibility. As a reminder, one person with the Delta variant transmits to at least eight others now. It’s an utter disaster. We have to use every mitigation approach in combination to reduce risk.
Indoor facilities for congregating people (such as schools) should budget for installing HEPA filters and UV light sanitization in their HVAC. Student cohorts per air intake area or placing desks with somewhat individualized air movement in a room can also help. If air exchange with the HVAC is inadequate, bringing in outdoor air should be considered. What is an adequate air exchange rate? The calculation is based on the volume of air in a room along with the number of people in a room. You can consult with an HVAC expert. OSHA recommends a minimum of four full air exchanges per hour, while hospital rooms should have six full air exchanges per hour. To increase air exchange, new ducts may need to be installed, which is no small feat. In the short term, adding UV light sanitization to an existing system would help. Stand-alone air purifiers with HEPA filtering can also help.
For my family’s allergies, I thought it was a good idea to use MERV-14 filters for our home’s central air unit. The additional strain to pull air through the dense filter probably wore out the fan motor prematurely, and we had to replace the whole system a few years ago. We ended up choosing a higher-end system with a built-in UV light system and the tech advised us to use a lower MERV rating for system longevity.
MERV ratings for air filters range from MERV-5 for the cheapest furnace filters at a discount store to MERV-11 as a pretty high standard for homes. Hospital operating rooms use MERV-17 and up. MERV-13 air filters can filter out about 90% of virus-laden particles, but it may be hard on your home HVAC. Plus, regular air filters simply can’t achieve HEPA filtration levels. HEPA filters are a different design, and they claim the HEPA designation by trapping particles down to 0.3 microns. Unless you have an HVAC system robust enough to use high MERV filters, you may need to rely on a stand-alone HEPA air purifier unit.
As for outdoor precautions, masks are necessary in a crowded area. Since there is far more air exchange, and the vertical air space is nearly infinite, outdoor activities are far safer than indoor. You need to pay more attention to wind direction and your position relative to the crowd. You want to be upwind from the others if possible. If you can smell a person’s perfume, body odor, or smoke, then you should wear a mask. Ten yards of distance is pretty safe. I visualize a much smaller glitter bomb. It doesn’t spew out as much glitter, the glitter disappears quickly in the UV rays of sunlight, and where the glitter travels is far more dependent on the wind direction.
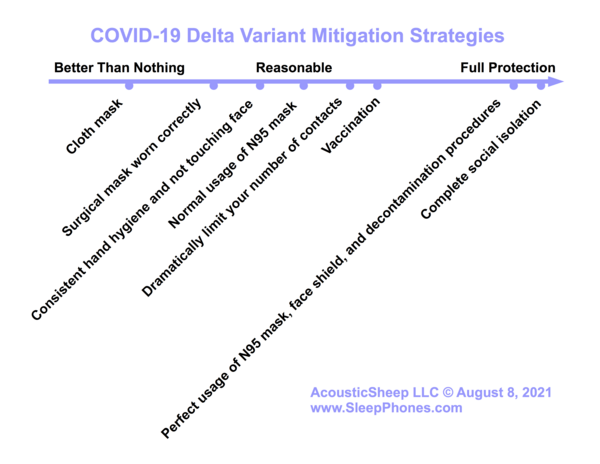
Mitigation measures in order of effectiveness
- Complete social isolation - zilch, nadda, utterly alone
- Perfect usage of N95 mask, face shield, and decontamination procedures, like experienced medical professionals
- Vaccination
- Dramatically limit your number of contacts - work from home, grocery delivery, homeschool
- Normal usage of N95 mask
- Consistent hand hygiene and not touching face
- Surgical mask worn correctly
- Cloth mask
There is no strong evolutionary pressure working to weaken this virus.
One of the most obvious evolutionary theories is that a germ that kills its host is ending its own life and therefore not very fit. Most viruses are most transmissible during the symptomatic stage. At the beginning of the pandemic, we based a lot of ideas and policies on SARS-CoV-1, the virus that caused SARS which stayed mostly in Asia in 2003. SARS was not contagious until after illness began. Once illness began, it was severe, with a mortality rate of 3%. That means that as soon as you were ill, you were sick enough to stay home. It was then that you were most contagious. Many of the people who caught SARS were healthcare workers who took care of ill patients. Through careful quarantines, contact tracing, and all of the mitigation measures you are familiar with, the world was able to stop SARS within eight months. “Only” about 8,000 people became sick with SARS. This is an example of a virus that was too lethal for its own good.
With COVID-19, you are contagious up to 48 hours prior to the start of symptoms. You could be inadvertently spreading the virus for two days prior to feeling ill. Once ill, the initial symptoms may not be severe enough to send you to bed. So you are still trying to tough it out and attributing the fatigue and discomfort to not sleeping enough, a migraine, or allergies. And there are just enough asymptomatic people spreading the virus for a full two weeks while engaging in normal social activities. The mortality rate is probably somewhere around 0.5%. While the illness isn't as severe as SARS, the end result is that more copies of this virus have spread to every corner of the world. Over 200 million people have had COVID-19. This virus is actually a far more “fit” virus from an evolutionary perspective.
The more lethal Delta variant spreads even more efficiently. One person infects eight people. In the beginning of the pandemic, one person spread to 2-3 people. Just like the previous versions, this variant spreads during the 48 hours prior to causing symptoms. Once the virus has gained so many new hosts, it has no incentive to keep that host alive to create more copies of itself.
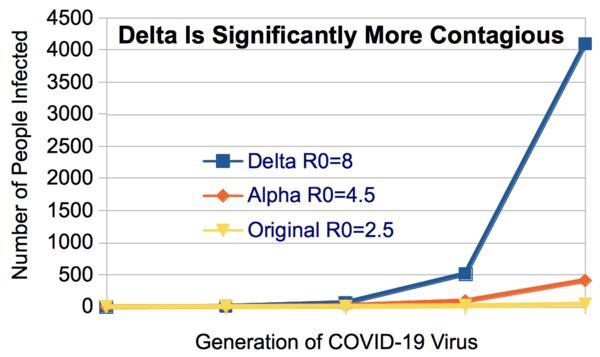
At the beginning of the pandemic, most experts believed that the virus would evolve to be less virulent, like the four other cold-causing coronaviruses we already know. But since this virus spreads so efficiently prior to causing symptoms, there is far less of an incentive to become less virulent.
Imagine that you were the virus with a stickier spike protein and more efficient replication within a human. You can spread to eight people prior to being detected rather than just two. It wouldn't matter if you happened to kill your host because you've already created more “children.” There is a sweet spot of lethality versus contagiousness, and that line is way too high for this virus to weaken based on the original theory.
Meanwhile, this evolutionary biology concept still holds: random mutations create variety. The more copies of a genome out there, the more mutations it will sustain. Mutations come about through errors in the replication process, cosmic rays hitting the genes, mutagenic chemicals, or other random events. It's like hitting the lottery. If you play one ticket, your chances of winning are extremely low. If you play 1 million tickets, your chances of winning are far greater. If “only” 8,000 people have a virus, the chances of it mutating are low. If 200,000,000 people have a virus, there will be many significant mutations. We are dealing with very significant combinations of mutations in the Delta variant.
Each new variant represents a whole new epidemic with different contagiousness, mortality, and risk profile. What's worrying me is the number of people now sick with Delta. It is entirely possible for us to have over 50 million people sick with Delta, and then we'll see mutations spin off from that deadlier virus. That means that we will likely have variants derived from Delta that are even worse. The more sick people, the more mutations. The key is to not get sick, but it becomes harder and harder as the virus evolves to be more contagious.
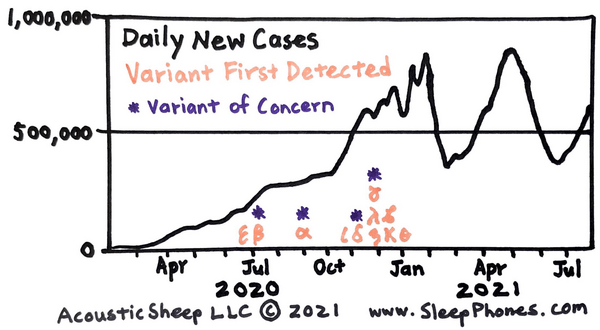
I previously wrote about where variants come from, and there are still two sources that are underreported in the popular news outlets. One is in immunocompromised people. They can partially fight off the virus, but since their immune system isn’t great, it doesn’t finish the job. So the virus mutates within the host under increasing selective pressures. One immunocompromised woman in Ireland had two significant mutation events over 82 days. On day 95, she contracted a new infection, which meant that she was infected with two slightly different COVID-19 strains. An immunocompromised man in Boston hosted an infection for 154 days during which the virus racked up 20 mutations. These patients were contagious the entire time they were ill.
The other underrated risk is in animal infections. Many viruses will stay within a species, not easily passed between species. Rabies is one exception. Influenza is another. Pigs and birds like chickens can catch the flu and spread it back to us. SARS-CoV-2, the virus that causes COVID-19, has been found in cats, mustelids (weasels, minks, otters, ferrets), and deer. The newer variants seem to be able to infect an even wider range of wild and domesticated mammals. Some sick minks were able to infect their caretakers at a mink farm in Denmark. They subsequently culled their entire mink industry in 2020. While transmission between species isn’t efficient, it’s still worrisome that there are so many animal reservoirs already for this new virus.
Vaccines really mess up epidemiological models.
The fact that the world is partially vaccinated with different vaccines with widely varying efficacy throws a whole new variable into the epidemiology and evolution of the virus. Obviously, vaccines greatly reduce the number of copies of the virus, so I'm all in favor of them. I give shots and teach medical students to give shots. I’m simply pointing out that trying to predict how many people will get sick over the next few weeks becomes harder when some of the population is vaccinated. Even the best vaccines (Pfizer and Moderna) are only partially (about 60%) protective for the Delta variant, so we don't have a good sense of cases that are asymptomatic but contagious. Now, there are probably proportionally more contagious people per confirmed case than before because the vaccines are keeping people asymptomatic. We don’t have firm statistics on this yet, since it’s still a developing situation. I’m worried that I’ll be an asymptomatic case who transmits it to my own young children.
I'm also worried that the virus is now under selective pressure to learn to escape the vaccine. The vaccine clearly helps to reduce viral load after the sixth day of illness. I would love to hear more from evolutionary biologists on the various evolutionary pressures from a virus's perspective. There is significant debate between medical and epidemiology experts on whether a worse variant will arise. There is no reason for the virus to weaken, so why wouldn’t it strengthen? Why wouldn’t it evolve to escape the vaccine?
To plan for the future, we need to know what is the most likely scenario, the worst case scenario, and the wildest plausible scenario. Having a wide range of experts weigh in from different angles will help map out potential pandemic paths over the next 1-2 years. Then we can plan ahead and gather the tools to deal with any situation. At the minimum, we need to increase vaccine production and distribution throughout the world. The vaccines should keep up better with the new strains. We must decrease disease burden to stop these mutations that will keep dragging this out indefinitely. Each new strain takeover will prolong the pandemic.
More than ever, it's important to face reality as it unfolds. What we went through in the winter of 2020 to stay safe was a dry run for what we should do again immediately. Holding on to old beliefs or being loyal to ideas is noble but not practical. I’m feeling the whiplash too, but this is reality. Anyone can learn more science and unlearn dogma. Science simply tries to quantify reality, and it's far from perfect. But the application of science in medicine has doubled life expectancy within two centuries, and babies die at 1/65 of the rate they did. It’s keeping nearly all vaccinated people from dying of COVID-19. As we discover more about the virus and as it evolves to replicate in us, we have to keep on adapting our behavior too. Protect yourself, protect your neighbors. Do everything you reasonably can to not get sick.
References
CDC ventilation advice
https://www.cdc.gov/coronavirus/2019-ncov/community/ventilation.html
Rhode Island department of health ventilation advice - good advice for the public, particularly those in charge at schools
https://covid.ri.gov/covid-19-prevention/indoor-air-circulation
Detailed ventilation advice for nursing homes
https://www.health.state.mn.us/diseases/coronavirus/hcp/hvac.pdf
Debunking the droplet versus aerosol five micron idea
https://www.wired.com/story/the-teeny-tiny-scientific-screwup-that-helped-covid-kill/
Denmark minks transmit COVID-19 to humans.
https://wwwnc.cdc.gov/eid/article/27/2/20-3794_article
Delta variant’s viral load is over 1000 times the original virus.
https://virological.org/t/viral-infection-and-transmission-in-a-large-well-traced-outbreak-caused-by-the-delta-sars-cov-2-variant/724
This pre-print that shows divergence between vaccinated and unvaccinated Delta variant viral load after the sixth day.
https://www.medrxiv.org/content/10.1101/2021.07.28.21261295v1.full-text
The Barnstable County outbreak led to indoor mask recommendations for vaccinated people.
https://www.cdc.gov/mmwr/volumes/70/wr/mm7031e2.htm
